Activate Your Population
Insignia Health’s PAM® Model Can Help Your Healthcare Organization Achieve Its Goals.
Our mission is to help everyone become a better manager of their own health and healthcare. To accomplish this goal, we empower healthcare professionals and organizations around the world with the tools and strategies to improve patient activation. This behavioral health model is anchored by the Patient Activation Measure® (PAM®) and our portfolio of validated activation measures. Over two decades of health research and PAM’s® practical application show that as patient activation increases, preventable utilization and costs decrease while health outcomes improve.

What is PAM?
It all starts with the Patient Activation Measure® (PAM®) survey. Both the 10- and 13-question versions are validated to assess the knowledge, skills and confidence underlying an individual’s health self-management and healthcare decision-making capabilities.
PAM Assessment & Scoring
The PAM survey produces a single score along a 100-point continuum that places individuals and populations into one of four unique activation levels.
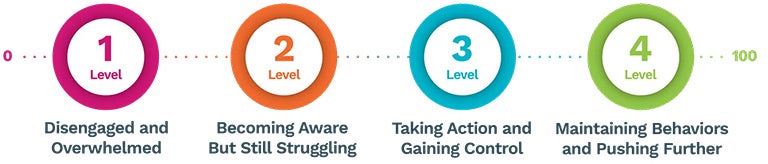
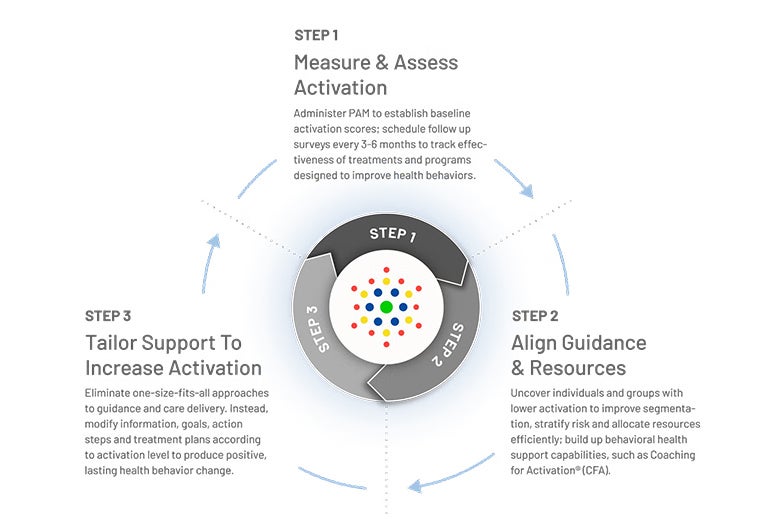
PAM Process & Engagement
Both PAM score and PAM level establish a foundation for analyzing an individual’s activation, as well as patient activation within associated groups and populations.
Changes in PAM score and level over time are expected and provide objective data for evaluating the effectiveness of treatment protocols, coaching guidance and allocation of health resources.
Benefits of Using PAM
Decrease Utilization Costs
Reduce Preventable Emergency Visits
Target Resources More Efficiently
Improve Patient Self-Management
Client Success Stories
As PAM scores increase, healthcare costs decrease
“In our study, if a patient’s PAM level increased one level, that was associated with 8 percent lower (Medicare claims costs over 6 months). For folks who improved two PAM levels, there was a 15 percent reduction in cost. When PAM level declined, the cost rose 9 percent for each level. In dollars, the average health care cost for people who remained at PAM level one was $12,700 a year, compared to $9,500 for people at PAM level 4. So, it’s significant. It can add up.”
— Ann Lindsay, Stanford University School of Medicine (SCOPE, 29 Oct 2018)

